It usually starts with the loud cries of one or two ladies which you can hear even if you are about 50 feet away from the site of incidence. Then you can see a gathering slowly building up around the bed from where the cries had originated. A doctor, a Nurse, one or two Interns can also be seen around the vicinity of the scene with emotion-less faces engaged in some kind of activity like giving a Cardio Pulmonary Resuscitation (CPR) or giving electric shocks to the patient with a Defibrillator or giving instructions to the Nurse which usually includes the words “Atropine” and “Adrenaline”. Then after a few minutes of hard work, the Doctor stops the CPR, looks at the monitor displaying straight lines with intermittent feeble sine waves. and examines the chest and the eyes of the patient. Then he walks out of the ward like a defeated warrior with his head held down and asking one of the male bystanders to accompany him. After explaining the reason why such interventions were done in the last one hour, the doctor declares that the patient is “no more”.
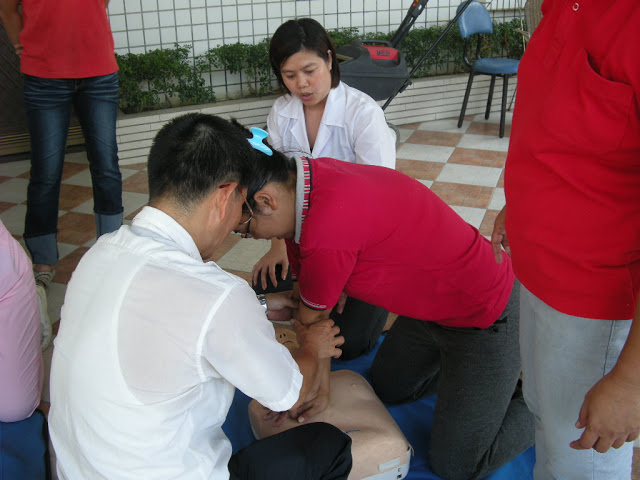 |
| Image Courtesy – Flickr I still remember the day when I got the call from the duty Nurse at 2 in the morning asking me to come to the ward as one of the patients who was in a serious condition due to Heart Failure had suddenly started gasping for breaths. It was during my Internship time at the Government Medical College, Kozhikode and I was the Ward Duty Doctor on that night at the Medicine Ward for Men. When I entered the Ward, there were already a group of men standing around the bed. The lady who was crying was sitting on the floor, outside the Ward and she was being consoled by another lady. I slowed down as I took my steps towards the bed. The patient was already on Oxygen inhalation, but there was no evidence of breathing. The Nurse was waiting eagerly for my instructions and to be honest I felt my tongue had swollen up and found it impossible to speak or make any kind of sound. One of the Nurses was giving a Cardio Pulmonary Resuscitation to the patient while the other was briefing me up about the patient’s condition. I couldn’t listen to what the nurse had just said because my eyes were fixed on the monitor which displayed big waves jumping simultaneously with the chest compressions. The only time when I had performed a CPR was on a dummy and I knew I will have to do it tonight on a dying man. I was not sure whether a CPR was required for this patient or not but I decided to do it nonetheless. When the nurse stopped giving the chest compressions, I took the ambu-bag which was connected to the oxygen line and gave two bag compressions. Then I climbed on to the patient’s bed and stood on my knees before giving the chest compressions, counting the same in my mind. I could feel a chest bone breaking under my hands as I was giving the chest compressions. When I stopped, I found my voice back again to order the nurse to give one ampule of Atropine and Adrenaline each to the patient. But even after giving multiple doses of those drugs, there was no cardiac activity displayed on the monitor except when the chest compressions were being given. I ordered to stop the resuscitation in order to check the patient for the vital signs of life. |
Nurse then asked me whether or not to give any more medicines for the patient. I could only nod a ‘no’ even though I tried hard to think what to do next. I took the patient’s Case File from the bedside table and started to read the latest orders. I knew the patient had Heart Failure because the Nurse had told me so when she first called me. There were many medicines written on the previous day’s Doctor’s Orders. With my other hand, I tried to feel the patient’s wrist pulse. I kept the Case File back on the table because my right hand fingers were drawing my attention to them. I tried to count the pulse for 10 seconds and could make it up to 18 beats. That means the patient’s heart was beating at about 100 beats per minute. And still the monitor on the table was showing straight lines! I was confused. What was happening?
I took the Stethoscope which was hanging around my neck and tried to auscultate the patient’s chest trying to listen to the fast beating heart. I placed the diaphragm of the Steth in almost every area where one could easily hear a Heart beating sound but I couldn’t. I thought maybe I should give an ampule of Adrenaline to boost the heart. What if there was still a chance to save this patient, I thought! I then tried to feel the Carotids of the patient with my same right hand’s index fingers. But this time I couldn’t identify any kind of pulse. I moved my hand towards the patient’s wrist and tried again and there was definitely a pulse palpable but a feeble one this time even though the rate was almost 100 beats per minute.
I thought I knew what was happening, and I needed to confirm it without anybody else noticing it. I wanted to make sure that the pulse which I had felt at the patteint’s wrist was mine. It should be and must be my pulse which I had felt against the wrist bones of the patient. In a vague motion, I brought one of my fingers towards my other hand’s wrist and it took only a few seconds for me to realise my folly. It was indeed my pulse. It was my heart which was beating at a high speed because of the sympathetic nervous system working properly at a nervous situation. The patient had expired clinically before my arrival and I felt a heavy weight pressing on my chest. I couldn’t save him. Maybe I was late to arrive and if I had reached a little earlier, I could have helped him and even saved him. The Nurse came close to me and told me whether an ECG (Electro Cardio Gram) was required to confirm the death or not. I thought about what the Nurse had just told for a moment and in a weak voice replied that it was not required.
I had just one more thing to do, confirm the brain death by identifying dilated pupils of the patient. When I lit up the torch and pointed it to the patient’s eyes, I could see the black pupils dilated to such an extent that the Iris was reduced to just a thin rim at the edge of the cornea. The more I stared at the blackness of the pupils, the more I was being drawn into the gloom.
I started to walk towards the Doctor’s room near the entrance of the Ward. I was being followed by a man who was the patient’s relative apparently.
“He is no more, and there was nothing more that we could do to save him”
After those words escaped my mouth, I thought it was a bit harsh and I should have declared the death of the patient in a little more diplomatic manner. But it was the by-stander’s response which amazed me.
“Don’t worry doctor sir, we were expecting this for months. Our doctor had explained to us yesterday night that his condition was a bit serious and that shifting to the Medicine Intensive Care Unit would be needed to save him. But the Medicine ICU had no vacant beds and the only option for us was to take him to a private hospital which we cannot afford.”
I had called the duty doctor at Medicine Casualty that night and informed him of the death of the patient. He asked me to write the death report in the Case File and told me that the patient was already in a bad condition and that resuscitation was not advised. It was that phone call which had lifted the weight of guilt from my chest. I took a deep breath and started to write the death report as instructed by the duty doctor.
I chatted with that man for another 30 minutes after finishing all the paper work. The time was around 3:30 am and still the thought of sleep had not occurred to me. I had just witnessed a human death and there was nothing much that I could have done to prolong the death, but still that guilty feeling haunted me for several days after that unforgettable night.